Remembering Valerie Guild, a tireless advocate for patients with melanoma
June 10, 2020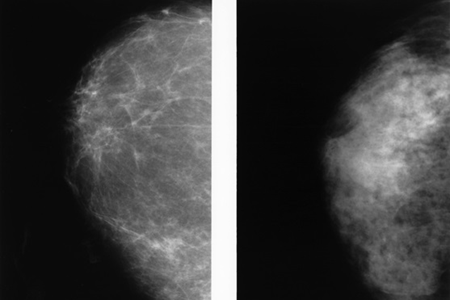
Trial Results: A 10-minute MRI proves useful in women with dense breasts at average risk of developing breast cancer
October 2, 2020Trial Results: For women with breast cancer in the TAILORx trial, cognitive decline from chemo was early and abrupt but did not get worse over time. Cognition also declined in the group on hormone therapy alone.

The Journal of Clinical Oncology recently reported that a subgroup of women on chemotherapy in the landmark TAILORx breast cancer treatment trial had an early and abrupt cognitive decline at three and six months following treatment, which leveled off at 12 and 36 months. The women received chemotherapy plus hormone therapy following surgery, to prevent the disease from returning.

“We found that chemotherapy produced early cognitive impairment that leveled off by one year and did not get worse over time,” says lead author Lynne I. Wagner, PhD, a professor of social sciences and health policy at the Wake Forest School of Medicine, pictured.
This study’s patient-reported data is meaningful to women with early breast cancer and the doctors who treat them. Dr. Wagner’s study also reports the loss of cognition in women who received hormone therapy alone.
“I think we’ve generally assumed that cognitive impairment is due to chemotherapy,” says Dr. Wagner. “Our findings tell us that hormone therapy may also play a role. Future research is needed to understand better how hormone therapy affects cognition in the context of cancer treatment and also how to treat this symptom.”
TAILORx is the first trial to look at cognitive impairment and health-related quality of life from the patient’s perspective. Dr. Wagner and her colleagues used questionnaires to capture data directly from patients, which gives confidence that the results accurately reflect women’s views on their symptoms and brain function.
Cognitive loss—or ‘brain fog’—involves memory problems, a lack of mental clarity, and difficulty keeping one’s focus. Cancer-related brain fog is common during treatment. This study dispels the idea that it is only from chemotherapy.
Women on Hormone Therapy Also Reported Significant Cognitive Impairment
The chemo group had more cognitive decline at three and six months after cancer treatment than the group on hormone therapy alone. However, at 12 and 36 months, the loss was not that different between the groups. This was not because the women who had chemotherapy improved, but rather because women on hormone therapy were also reporting a loss of cognition, although the pace of their decline was slower and more gradual.
Dr. Wagner says: “The persistent cognitive impairment reported in both groups identifies the need for research to understand this distressing symptom better.”
Cognitive Function Did Not Return to Pre-Treatment Levels in Either Group
Another key finding from TAILORx is that women’s cognitive function did not return to pre-treatment levels regardless of the treatment they received.
 “It is concerning that women’s cognitive function did not return to pre-treatment levels after finishing chemotherapy, and neither did the group with hormone therapy alone,” says Mary Lou Smith of the Research Advocacy Network, and chair of ECOG-ACRIN’s Cancer Research Advocates Committee, pictured. “This patient-reported data speaks to the need for prevention research or at least research to develop treatment strategies that lessen the severity.”
“It is concerning that women’s cognitive function did not return to pre-treatment levels after finishing chemotherapy, and neither did the group with hormone therapy alone,” says Mary Lou Smith of the Research Advocacy Network, and chair of ECOG-ACRIN’s Cancer Research Advocates Committee, pictured. “This patient-reported data speaks to the need for prevention research or at least research to develop treatment strategies that lessen the severity.”
Other Findings
Many have questioned whether cancer-related cognitive decline is due to aging, menopausal changes, or as a sign of anxiety and depression. These findings did not differ based on age. Dr. Wagner and colleagues observed the same amount of cognitive changes among women under 50 years old, 51-64 years old, and 65 years and older. They saw the same pattern of results for women who were pre-menopausal as those who were post-menopausal. Neither anxiety nor depression could account for the cognitive changes they observed.
About TAILORx and Genetic Testing
The groundbreaking TAILORx trial found no benefit from chemotherapy in 70% of a group of women with HR positive, HER2 negative, node-negative breast cancer: older than 50 years and with an Oncotype DX Recurrence Score® of 11–25; any age with a recurrence score of 0–10; and 50 or younger with a recurrence score of 11–15. These results, published in 2018 in the New England Journal of Medicine, give clinicians high-quality data to personalize treatment for women with early breast cancer.