Trial Results: For women with breast cancer in the TAILORx trial, cognitive decline from chemo was early and abrupt but did not get worse over time. Cognition also declined in the group on hormone therapy alone.
October 2, 2020
Ongoing Trial: In the TMIST mammography trial, nearly 20% of the volunteers are Black women, thanks to a successful recruitment strategy
October 2, 2020Trial Results: A 10-minute MRI proves useful in women with dense breasts at average risk of developing breast cancer
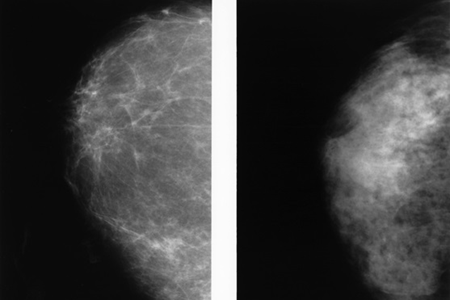
A side-by-side of two normal mammograms showing the difference between a fatty breast (not dense) (left) and a dense breast (right).

By Christopher E. Comstock, MD
When screening women with dense breasts and at average risk of developing breast cancer, my ECOG-ACRIN colleagues and I found that a 10-minute breast MRI exam detected significantly more—almost two and a half times as many—breast cancers than 3-D mammography. We also found that the short breast MRI was well tolerated by women, with very few side effects. Our findings, from the EA1141 clinical trial, were recently published by the Journal of the American Medical Association and are a sign of progress for women with dense breasts.
Despite current screening methods, over 40,000 women die each year from breast cancer. The ability of mammography to detect breast cancer is limited in women with dense breast tissue. Having dense breasts is quite common; in fact, about half of all women over the age of 40 have dense breasts.
Breast MRI is a screening test that uses radio waves to capture images following intravenous injection of contrast dye. Because it is not limited by breast density, MRI offers the highest cancer detection rate of all breast imaging tests. However, breast MRI is more expensive than a mammogram, takes longer to perform (45 minutes compared to about 15 minutes for a mammogram), and requires an injection.
The EA1141 study looked solely at 1,444 women between the ages of 40 and 75 with dense breasts and at average risk of developing breast cancer. It provides promising results for using the shortened MRI in this group of women. My ECOG-ACRIN colleagues and I are also conducting another much larger breast cancer screening trial, called TMIST, where we are seeking ways to personalize screening for all women (not just those with dense breasts).
Although most evidence exists for using MRI to screen the small proportion of women at very high risk of breast cancer, this new study adds to the growing body of evidence that the higher sensitivity of MRI is also useful for women with dense breasts at average risk.
Although MRI is undoubtedly the most sensitive test for detecting breast cancer, it is not currently used to screen the large number of average-risk women with dense breasts due to its high cost and time to perform. The 10-minute MRI reduces the complexity and cost of MRI by shortening the time it takes to perform and interpret the exam. The EA1141 study results will hopefully give far more women access to this powerful tool in the fight against breast cancer.
While these early results are promising, we need further studies to evaluate the cost-effectiveness of widespread screening with shortened breast MRI and its impact on reducing breast cancer mortality. Currently, only a few centers offer abbreviated breast MRI, and insurance does not cover the procedure. We hope that the EA1141 study results will encourage more centers to provide this new test and that insurers will see its benefit to improve early detection of breast cancer.
Dr. Comstock is attending radiologist at Memorial Sloan Kettering Cancer Center, imaging chair for ECOG-ACRIN’s Breast Cancer Committee, and the lead investigator for the EA1141 clinical trial.